THE DOCTOR'S BAG
the blog about medicine and surgery in the 19th century
Keith Souter aka Clay More
The 19th century saw monumental changes in medicine and surgery as the Germ Theory of disease and the discovery of the disease-making potential of micro-organisms gave doctors an understanding of how infections were caught. The development of aseptic surgery gave people a fighting chance of surviving operations and the infections that developed afterwards. Yet it would be public health measures based on hygiene, sanitation and fresh water supplies that would reduce mortality rates in towns and cities.
Epidemics were a problem for cities as the century advanced. With industrialisation, people moved to the cities to gain employment. Overcrowding in unsanitary conditions created the right conditions for infectious diseases to develop and pass rapidly through the population.
In London in 1854 there were 14,000 cases of cholera with 618 deaths. In the USA there were three cholera epidemics in the 19th century.
Yellow fever was a huge problem in the northeast states between 1793 to 1805. Then in the first half of the 19th century it hit the southern states, to reach a peak in the 1850s.
Infections and disease during the Civil War
The war had a devastating effect on the country, but there were more deaths from disease than from battle. This may seem surprising, until you consider that the assembling of armies with men living in close contact, with limited hygienic precautions, poor sanitary standards and sometimes inadequate nutrition and water.
Wounded Union soldiers being tended near the Marye house in Fredericksburg, Va, after the Battle of Spotsylvania
According to Medicine of the Civil War by Paul E Steiner, published by the National Library of Medicine, there were almost 3 million enlistments to the Union Army and between 1.3 - 1.4 million to the Confederacy.
The deaths from various causes were highly significant:
UNION:
In battle 110,070
Disease 224,586
Accidents, suicide, etc 24,872
Total 359,528
CONFEDERACY:
In battle 94,000
Disease, etc 164,000
Total 258,000
The total deaths in battle amounted to 204,070, compared to 388,586 deaths from disease. Effectively, diseases caused almost twice as many deaths as did actual battle.
Figures for admissions to hospital for the Confederacy are not available, but for the Union:
DISEASE
|
CASES
|
DEATHS
|
Typhoid
|
75,368
|
27,050
|
Typhus
|
2,501
|
850
|
Typho-malarial fever
|
49,871
|
4,059
|
Acute diarrhoea
|
1,155,266
|
2,923
|
Chronic dysentery
|
25,670
|
3,229
|
Syphilis
|
73,382
|
123
|
Gonorrhoea
|
95,833
|
6
|
Scurvy
|
30,714
|
383
|
These sickness figures show that some conditions had an alarmingly high mortality rate. The mortality rate for typhoid was over 35 per cent of cases. Typhus was less common, but had a mortality rate of 34 per cent. Typho-malarial fever, a common diagnosis, which showed the lack of understanding about the conditions of typhoid and of malaria (which are separate conditions) and the non-specificity of diagnosis, had a mortality rate of 8 per cent. Other conditions like acute diarrhoea caused huge numbers of cases, throwing a terrific drain on resources and taking so many men off the field of battle, without having a high mortality rate. Add to that the huge number of men who had to be treated for the venereal infections and the men who would have been very ill from scurvy, caused by lack of vitamin C and you can see how disease was just as much a dangerous enemy as the foe on the opposing side.
The figure are not complete, of course. There would be the added cases of tetanus and gas gangrene, both potential complications of being wounded and lying on a muddy battlefield where the wounds would be likely to get infected from organisms in the soil.
The Union, which lost control of the battlefields in the early stages battles took the greatest number of casualties with infected wounds, but gradually both sides developed ambulance services and field and general hospitals so the wounded fared better in the later stages of the war.
Surgeon General William A Hammond (1828-1900) was in charge of the Union medical services at the start of the war, but fell from grace and was court-marshalled on trumped up charges against him.
The Confederacy's medical services were overseen by Dr Samuel Preston Moore (1813-1889). He was able to build up the southern medical corps with comparatively little interference.
Dr Samuel Preston Moore - surgeon general of the southern medical corps
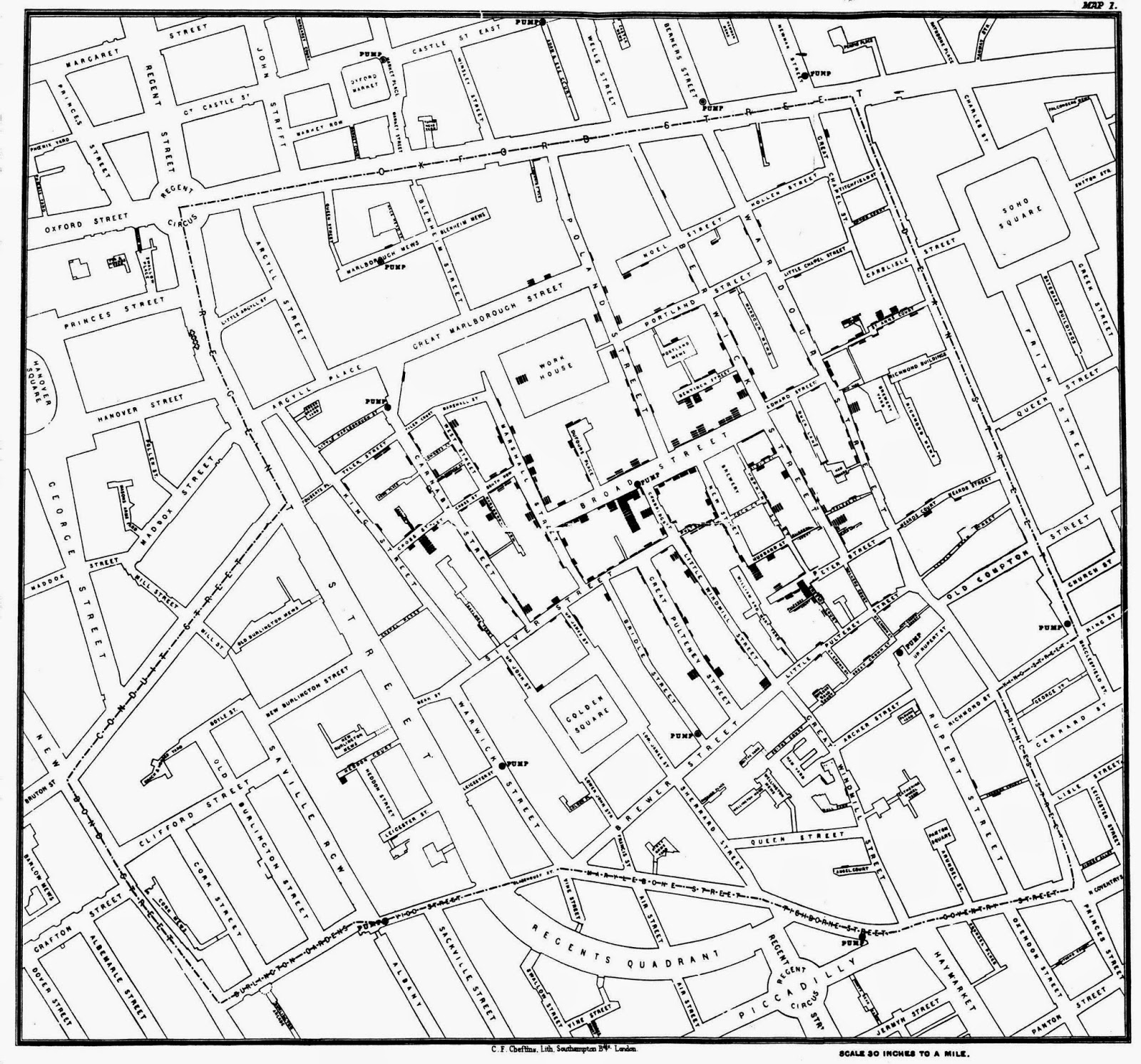
The 1854 London Cholera Outbreak and the Broad Street Pump
A very severe outbreak of cholera broke out in the Soho area of London in 1854. At the time the medical opinion was that cholera was caused by bad air and that one could acquire a miasm from this, that caused the disease. The idea that it was due to an infecting organism had not occurred to anyone.
Dr John Snow (1813-1858) did not accept this idea and wrote an essay On the Mode of Communication in Cholera in 1849, in which he postulated that cholera entered the body through the mouth, not through inhaling bad air.
Part of the cholera death map of Soho in London, pinpointing the Broad Street Pump (centre of picture)
During the outbreak of cholera in 1854 he performed the first ever epidemiological survey. He charted all the cases of cholera and all the deaths, to produce a cholera death map. He was able to deduce that the commonality was that all deaths had occurred in an area supplied by a water pump in Broad Street. The water from it had been contaminated by a cracked sewage pipe. He had the handle of the pump removed so that it could not be used and the number of cases started to drop straight away.
Dr John Snow was also a pioneer in the development of anaesthetics and gave chloroform to Queen Victoria during one of her labours. Because it was so successful for the queen anaesthetics was given a much-needed boost in popularity.
Once the Germ Theory became accepted, doctors began the hunt for micro-organisms in all of the infectious diseases. Gradually, it became clear that there were various modes of transmission of these infections.
Airborne transmission
The organisms are transmitted in droplets from coughs and sneezes. These droplets are inhaled by someone else, who develops the illness.
Diseases spread in this manner:
- The Exanthemata (the diseases characterised by a distinctive rash) - measles, rubella (German measles), chickenpox, smallpox, scarlet fever.
- Mouth and throat infections - diphtheria, tonsillitis, mumps, herpes stomatitis.
- Respiratory tract infections - pertussis (whooping cough), influenza and other respiratory virus infections, pulmonary tuberculosis.
- General - meningococcal and staphylococcal infections.
Intestinal
Infection present in the bowel excreta of a case or a carrier (someone who has the infection, but who has no symptoms) is ingested by a previously uninfected person. This transmission may be immediate and direct, via infected fingers and hands, eating utensils, clothing, toilets, or indirectly via infected food or water.
Diseases spread in this way include - typhoid and paratyphoid, salmonellosis, dysentery, cholera, gastroenteritis, poliomyelitis, viral hepatitis.
Direct contact
This is from person to person by skin contact. These are mainly cutaneous (skin) conditions like impetigo, scabies and cowpox. But other serious conditions like anthrax can also be transmitted by direct contact.
Venereal route
These are infections by sexual contact. This includes syphilis, gonorrhoea, lymphogranuloma venereum, herpes genitalis and HIV.
Insect or animal route
Infections transmitted by animal and insect bites include malaria, trypanosomiasis, typhus and rabies.
Other infections like Weil's disease (leptosprosis icterohaemorrhagica) is excreted in infected rat's urine and contaminates stagnant water. This could later penetrate the skin of a bather. It causes jaundice and blood in the urine.
Tetanus can be contracted from the faeces of herbivorous animals which has contaminated the soil.
Other diseases can be transmitted by animals' milk. The bovine form of tuberculosis, for example can be transmitted by drinking infected milk.
Common infectious diseases of the 19th century
The following diseases were all common. The years that the infecting organisms were first identified have been included, where known.
Cholera
This is an infection of the small intestine caused by Vibrio cholera, a type of bacterium, which was discovered by the Italian anatomist Filippo Pacini in 1854. He did not realise that it caused cholera. This was concluded by Emile Koch in 1884.
It is transmitted by drinking or eating infected food or water. The incubation period is 4 -12 hours, so it is a fast-spreading disease.
It causes profuse diarrhoea and vomiting, abdominal colic and leg cramps. Fluid loss from the diarrhoea, classically described as 'rice-water stools', can produce a state of shock within 24 hours. Kidney failure can be a complication in those who recover. Death can occur within 24 hours to a few days without hydration.
The treatment depends on adequate fluid replacement. Nowadays this is with intravenous fluids. Some antibiotics are effective, but hydration is the essential.
Prevention depends on strict hygiene, the provision of pure water and safe sanitation.
Diphtheria
This used to be a common childhood disease, but is now uncommon, thanks to vaccination in childhood. It is still a danger however to those children who are un-immunised. It is caused by Corynebacterium diphtheria, discovered by Edwin Klebs and Freidrich Loffler in 1884. It is sometimes known as the Klebs-Loffler bacillus.
Diphtheria causes the formation of a grey membrane of exudate in the throat, which may completely obstruct the airway. It is characterised by high fever, increasing drowsiness and difficulty breathing.
When people were treated they were to be kept lying down and not sat up, because the bacterium can spread to the heart to cause damage to the heart. This would produce a myocarditis, or inflammation of the heart. This makes abnormal heart rhythms develop at a point between 10 and 21 days. These could be fatal. Recovery would not be considered complete until after that danger time.
Later complications at the third week up to the seventh week could affect the nervous system to paralyse muscles. This could affect speech or eye movements or the swallowing mechanism. Recovery would eventually be complete.
The membrane and respiratory problems could cause suffocation and it could be necessary to perform the operation of tracheotomy, an operation to make a hole in the airway and insert a metal tube to by-pass the obstruction until the membrane resolved.
An antitoxin was developed by Emil von Behring in 1890. This would be given by injection. Nowadays all children are immunised against the disease as babies.
The mortality rate for diphtheria was 5-10 per cent. In 1881 and 1887, nearly 5,000 people died from diphtheria in the city of New York.
The tracheotomy operation
This is an operation to make a hole in the trachea. The word is sometimes used interchangeably with tracheostomy, although to be correct tracheostomy refers to the hole that is made, while tracheotomy is the operation to make the hole.
There were various methods of doing the operation, sometimes referred to as a high or a low tracheotomy. The easiest way would be to do an operation that is still used today in emergency rooms, involving making an opening in the cricothyroid membrane, a soft tissue just below the Adam's apple in the throat.
To do the high or low operations the following instruments would be required: scalpel, forceps, the more slender the better, 2 pairs of fine toothed forceps, a sharp hook. A tracheotomy tube with a retaining cuff, tongue forceps and gag.
The patient's head would be steadied on a sandbag, arranged so that the throat could be steadied. It is important to maintain the midline, so that the surgeon knows precisely the anatomy that he is going to work through.
To perform an emergency operation in the Old West, an incision would be made precisely in the median line of the neck, about one inch in length. The cricothyroid membrane would be identified and an incision made in it. Then the tracheotomy tube would be inserted. A fine feather would have been used to clear the tube.
Tracheotomy - the cricothyroid membrane is indicated by ll - an incision was made and the tube inserted
Upon making the tracheotomy there would be a noisy rush of air entering and escaping though the wound. The child would cough, expelling mucus and the grey membrane. It would be life-saving.
In my novel The Doctor, based on events in the life of Dr George Goodfellow, published by Western Fictioneers Library I have the good Tombstone doctor perform an emergency tracheotomy upon a patient lying on pool table.
Smallpox
This widely feed disease could affect people of all ages. It had a very poor prognosis in young children.
It is caused by either the Variola major or the Variola minor virus. The Variola word means spotted or pimpled. Variola major caused a much more serious disease. It is now considered an eradicated disease by the World Health Organisation, thanks to the success of the smallpox vaccination programme.
After an incubation period of 11-12 days the rash of smallpox would develop. It had several clinical patterns, but effectively, they all produced a rash with multiple small blisters covering the body. They would burst and form scarring crusts.
There was no effective treatment, merely supportive care, adequate nutrition and hydration.
The mortality rate in the 19th century was high. Depending upon care facilities, the previous health of the population affected and a good measure of luck, it could kill 20 to 60 per cent of cases.
It would leave scarring and it caused a third of the blindness of the day.
Typhus
This was a disease that as we saw earlier caused significant mortality. It is caused by rickettsia bacteria transmitted by lice, leas, ticks and mites. It is the name given to a number of related illnesses. The insects are carried from person to person or are brought from other animals.
Epidemic typhus was called camp fever, jail fever or war fever. Overcrowding in unsanitary conditions encouraged its spread.
The incubation period was about ten days, after which the person develops headaches, loss of appetite, malaise, raging fever, chills and nausea. Four to six days after the start a rash develops over the whole body.
The fever would continue until about the 12th day, then recovery would take place on about day 14.
Left untreated the circulation becomes sluggish and thromboses may occur, leading to areas of gangrene on the digits, genitals, nose and ears. Pneumonia or kidney failure, or both, could develop. The course may be progressively downhill, ending in death.
It is effectively treated with chloramphenicol and tetracycline antibiotics nowadays, but in poor sanitary conditions, overcrowding, as occurs in disaster areas around the world, and without medical facilities the death toll can still be high.
A vaccine was developed during World War ll.
Yellow Fever
This viral disease is spread by the bite of infected mosquitoes. Humans and other primates can be affected. The usual mosquito involved is called Aedes aegypti. The virus is an RNA Flavivirus.
The incubation is 3 to 5 days, when symptoms begin. These include headache, severe muscle pains, high fever, nausea and vomiting. The condition usually resolves after 3 or 4 days, but 15 per cent go on to develop more severe symptoms, including jaundice, whence it gets its name, and bleeding from the nose, eyesore stomach. Half of those suffering the severest form will die.
It had various names - yellow plague, bronze john or yellow jack.
Yellow fever caused many deaths in ares of the world prone to it during the 19th century. These were mainly South America and Africa, where it is still a problem. The USA also was hit by numerous major outbreaks.
Dr Wilbur Sawyer developed the first effective yellow fever vaccine in 1931. A safer vaccine was produced in 1937 by Dr Max Theiler. In 1951 Dr Theiler won the Nobel Prize for Medicine for the yellow fever vaccine. For some unaccountable reason Dr Wilbur Sawyer was not also given the prize.
The vaccine makes the disease entirely preventible and it is given 10 days before entering a yellow fever area. Protection will last for 10 years.
Poliomyelitis
This infectious disease mainly affects children, but is now preventible through vaccination. It attacks the central nervous system, often resulting in a child waking to be partially or totally paralysed. Bed rest was the only treatment, until people discovered the need for physiotherapy. When then respiratory muscles were affected people were left unable to breathe without assistance, so the 'iron lung' was developed in 1928. This was a large cylinder in which the person lay. Controlled negative pressure inflated and deflated the chest to assist breathing. Earlier wooden versions had been developed worked by hand cranked bellows.
The vaccine against polio was developed by Jonas Salk in 1952.
Malaria
We briefly referred to malaria in the post on Fevers and Pest Houses. Hippocrates described in beautifully, differentiating the different types of fever associated with it. He thought that it was caused by bad air, which thought persisted until the 19th century in the name 'mal' 'aria', literally meaning 'bad air.'
Malaria is still the most common and serious of all the tropical infectious diseases. It is still endemic in large areas of the Pacific, Southern Asia, Central and Southern America and Africa. If it is not treated promptly it is frequently fatal.
The author had experience of treating malaria while working in an infectious disease hospital in Southern India back in the 1970s, while still a medical student.
Malaria is caused by protozoal parasites of the Plasmodium group. They are spread by a single bite of an infected Anopheles mosquito. There are many different Plasmodium parasites, but only five of these cause the disease in humans.
Three of these, Plasmodium vivax, Plasmodium ovale and Plasmodium malaria cause a relatively benign illness with tertian (alternate day) fevers, or occasionally quartan (every third day) fever. Plasmodium falciparum causes a more serious type of malaria, which used to be called 'malignant malaria' or 'blackwater fever.' In this the kidneys are affected and broken down blood appears in the urine to make it appear extremely dark, like black water. This is called haemoglobinuria.
The different types of fever, which Hippocrates described, relate to the life cycle of the malarial parasites in the blood. The condition causes the variable fevers mentioned above, chills, headaches, abdominal pains, muscles pains, vomiting and diarrhoea and general prostration. The spleen can become extremely enlarged, as outlined in the post on Fevers and Pest Houses.
In the 19th century before the malarial parasite was discovered it was found difficult to differentiate it from typhoid fever, hence it was often called typho-malarial fever. From experience, I can attest to the difficulty of distinguishing them on purely clinical grounds. Fortunately, we now have blood tests, which will distinguish them, as the parasites will be found in the blood.
Sir Ronald Ross (1857-1932) was a British doctor working in India. In 1895 he discovered the Plasmodium parasite in the stomach of the Anopheles mosquito. He conducted research over two years and managed to cultivate mosquitoes from eggs, effectively elucidating the life cycle of the mosquito. He then had a volunteer patient who already had malaria and managed to get them to bite him. When they did they sucked up blood into their stomachs. He examined them over the following days and was able to see how the parasites developed in their stomach. He had found that the mosquito was an important link in the chain.
Notebook belonging to Ronald Ross, describing the parasites from the mosquito stomachs he had seen down the microscope
He realised their significance and wrote a poem to his wife about them:
This day relenting God
Hath placed within my hand
A wondrous thing; and God
Be praised. At His command,
Seeking His secret deeds
With tears and toiling breath,
I find thy cunning seeds,
O million-murdering Death.
I know this little thing
A myriad men will save.
O Death, where is thy sting?
Thy victory, O Grave?
He knew that he was on the verge of a discovery that could save countless lives. By attacking the life cycle of the mosquito which develops in stagnant water, the sort of surroundings that Hippocrates had thought produced 'mal' 'aria,' it was possible to reduce the number of cases.
Sir Ronald Ross, the discoverer of the malarial parasite
In 1902 he was awarded the Nobel Prize for medicine.
Quinine was used to treat malaria since the 17th century. The bark of the cinchona tree (quina quina) was called Jesuit's bark, Cardinal's bark or Sacred bark. It was discovered by a Jesuit priest in South America in 1630, although their are legends about it being used by the local native population before then.
The introduction of quinine to Europe involves the Spanish Countess of Chinon, who contracted malaria in Peru. She was given a draught concocted from the bark of a tree and recovered. When she returned to Spain she introduced quinine to Europe in 1638. It was known as the Countess's powder. In 1742 the botanist Carl Linnaeus called the tree Cinchona in her honour.
Supplies of quinine were critical during the Civil War. The Union Naval blockade cut off supplies to the Confederacy, who were forced to find alternatives. Dr John Chisolm, the inventor of the Chisolm inhaler was tasked with doing this, which he set about quite ingeniously, as described in the post on him.
The great writer and preacher John Bunyon wrote:
Yet the captain of all these men
of death that came against him to take him away, was the consumption, for it
was that that brought him down to the grave.
Consumption was a great catch-all diagnosis. It would have included all sorts of degenerative disease, including many cancers and respiratory conditions that could not be specifically diagnosed in days gone by. Nowadays we know it as tuberculosis.
Tuberculosis is highly contagious infectious illness cause by a bacterium called Mycobacterium tuberculosis. It exists as two main strains, the human and the bovine. The main source of infection of the human strain is from the respiratory tract of a person with the disease. Transmission takes place by droplet spread, in other words coughs and sneezes.
The bovine form is contracted from ingesting infected milk or dairy products.
Even today, according to the World Health Organisation, WHO, tuberculosis is second only to HIV as the greatest killer worldwide due to a single infectious agent.
Common symptoms of active TB are cough with productive sputum, sometimes with blood, general malaise, chest pains, weakness, weight loss, fever and night sweats.
Antibiotics are the treatment nowadays for active cases. A vaccine called BCG, which stands for the 'Bacillus of Calmette and Guerin,' is available, but is not much used in the USA. It is often given to young children in Europe and in countries where it is a problem.
In the 19th century people often sought better climates to cope with their illness, hence many people suffering from it would head to the American southwest. Later, people who were very ill would be admitted to a tuberculosis sanatorium.
Doc Holliday famously had tuberculosis and moved west, to Dodge City and Tombstone where the climate and the lifestyle suited him. One of the doctors he consulted in Tombstone was Dr George Goodfellow, the surgeon to the gunfighters. He had nothing to offer him, since the causative organism was not discovered by Robert Koch until 1892. Doc Holliday died in Colorado in the Hotel Glenwood. Many stories say that he died in a tuberculosis sanatorium, but the Glenwood Springs Sanatorium was not built until 1896, 9 years after his death.
Another person who had apparently travelled west because of her consumption, was the singer and actress Dora Hand. She went to Dodge City in 1878 and became extremely popular. Sadly, she was shot to death when a cowboy named Spike Kenedy fired into the cabin she was sleeping in, because he believed that the mayor, 'Dog' Kelley was sleeping there. A posse was formed, the members including Wyatt Earp, Bat Masterson and Charlie Bassett. They caught him, wounding him in the process, but he was later acquitted, because there was deemed to be insufficient evidence. His father, Mifflin Kenedy had come to the young cowboy's rescue, as he had done before.
Dora Hand was interred in Boot Hill.
Variolation to vaccination
The discovery of vaccination has been one of the greatest advances in the history of medicine. The ancient Greeks had observed that people who contracted and survived smallpox did not get a second attack. It seemed that once you had the disease you had protection.
The Chinese presumably noted the same thing and tried to do something to produce a milder form of the illness. They discovered a process called variolation in the 10th century AD. It was in effect a primitive form of vaccination against smallpox. It involved exposing healthy non-infected people to the scabs of people who had smallpox. These were either put under the skin or inhaled up the nose. Variolation certainly seemed to protect against smallpox by inducing a milder illness. Even so, it was not completely safe. It could still kill, although not as often as smallpox did.
The Chinese practiced this for centuries, but it was not until merchants from Turkey brought it back centuries later that it spread to Europe. This was very welcome, since the disease at that time killed one in five people during epidemics.
In 1717 Lady Mary Wortley Montague (1689-1763), the wife of the British Ambassador to Turkey heard about variolation in Constantinople. So impressed was she, and so convinced of its efficacy that back in Britain she and the princess of Wales persuaded the authorities to permit a hazardous and unethical experiment. A group of convicted prisoners and orphaned children were given variolation, by having scabies scabs inserted under their skin. A few months later they were deliberately exposed to smallpox. None of them contracted the disease and the procedure was deemed to be safe. Several members of the royal family were inoculated, the result being that variolation became fashionable.
Variolation was introduced to America by African slaves. Cotton Mather, a Boston theologian and Puritan minister learned about variolation from his slave, whom he had christened Onesimus. Mather discovered that other slaves had also been variolated and he found some literature that referred to the method employed in Turkey. When an epidemic of smallpox hit Boston he was able to encourage variolation, with good effect.
In 1796 Dr Edward Jenner (1749-1823) an English physician and scientist discovered vaccination.
He had been inoculated by variolation as a child. Unfortunately for him, he suffered complications from the process for the rest of his life, but wondered if there could be a more effective way of giving protection against the condition.
Dr Jenner noticed that cow maids often contracted cowpox, a much milder condition than smallpox, but did not contract smallpox. He researched this and found that by inoculating pus from the lesions of cowpox onto a healthy person it gave them protection against smallpox.From this he established the principle of vaccination, which has since saved millions of lives.
In the 1880s, with the development of the Germ Theory a greater understanding of how micro-organisms caused disease was developed. This helped enlightened researchers to look for ways of curbing the ravages of these infectious illnesses. In 1884 Louis Pasteur discovered the rabies vaccine and put it into practice in humans in 1885.
In 1890 Emil von Behring added to the success story of vaccination when he discovered the diphtheria vaccine and the tetanus vaccine. Then the Japanese physician Shibasaburo Kitasato dissevered the antitoxins of both diphtheria and tetanus, when he demonstrated that animals could be protected by injections of these antitoxins.
In the 20th century vaccination programmes were developed around the world against many of the dangerous infectious diseases, and in 1955 polio vaccination dramatically reduced the suffering from poliomyelitis. Now this disease is very rare.
In 1980, one of the greatest success in medicine was achieved when theWorld Health Organisation declared that smallpox had been eradicated.
***
Some of Clay More's latest releases:
- a novelette- novella
Sam Gibson used to be a lawman, until the day he made a terrible mistake that could never be taken back. Since then, he has alternated between wishing there were a way he could redeem himself and believing he deserved punishment.
He’s about to get both…
REDEMPTION TRAIL
And his collection of short stories about Doc Marcus Quigley is published by High Noon Press
Available at Amazon.com:
And his latest western novel Dry Gulch Revenge was published by Hale on 29th August.














Thank you for adding to the understanding of these diseases that were so much a part of out history. I always look forward to my monthy lesson. There was a girl in my school who had polio and I remember her using braces and crutches to walk, but she eventually ended in a wheelchair. Doris
ReplyDeleteThanks, Doris. Yes, it is an extremely debilitating condition. We have to be grateful for the development of the polio vaccine.
DeleteI remember getting the sugar cube, along with all my siblings. I believe even my parents took it, but I was so young I can't recall...
DeleteAh the magic sugar cubes, when we were allowed to use them.
DeleteDr. Keith,
ReplyDeleteWOW, what a lot of information! As a young man, I first read a written piece by John Steinbeck the writer, stating that in training camps for the military, many soldiers are exposed to illnesses, get sick, and die. I myself, at Fort Knox Kentucky basic training, contracted bacterial meningitis. Many of the young men died and why I survived I don't know. With a temperature of 106, blood bursts from veins and forms hard lumps and stretch marks. After recovery, skin sheds like that of a snake. Those who recovered suffered paralysis of some form. I myself suffered nerve damage and tremors but for some reason the Army kept me, (I could and can shoot straight between the shakes). I am positive some IQ points were lost in the process. Perhaps that explains a lot!
Like I said so many times about your articles---they are so thorough---but so hard to contemplate all these serious and dangerous diseases which any one of us could get and die from. SCARY STUFF!!
Glad you're the doctor and not ME! Just by your demeanor, I am CONVINCED you are a good doctor indeed.
Once again, thank you?
Thank you, Charlie. Meningitis is indeed a horrid condition. I am glad that you recovered so well.
DeleteWe really still know so little about many of the pathogenic illnesses. We can't predict the course of them, or who will do well and who may suffer a more severe attack. All this despite Hippocrates saying that doctors should cultivate the art of prognosis.
Thank you for your kind words!
Keith, what a wonderful wealth of information! And much of this will be available in your BOOK! YAY! I don't know how you are able to remember so much, but I certainly do envy you, carrying all that knowledge around in your head. Like Charlie, I'm convinced you're a good doctor, too. You truly found your calling in life and you are wonderful at it!
ReplyDeleteCheryl
Thank you, Cheryl. You are too kind. And thank you about the book. I am looking forward to it and hope that my fellow writers may find it of some use.
DeleteGood thing you're coming out with a book. Easier than hunting up all this in old blog posts when research is necessary. :-D
DeleteAnother fabulous post, Doc. Can't wait to meet you and the other WFs in St. Louis!
ReplyDeleteI just came across this great article and see the blog is followed by familiar writers...I'm researching typhoid in Bisbee, AZ, 1886-1889 without much luck. Jane A. Delano, RN and FDR's cousin was there to help and went on to develop the American Red Cross Nursing program. Does this ring any bells? I have Red Cross material and will search it further but would welcome any clues at Arletta_dawdy@yahoo.com Thank y'all..
ReplyDeleteThank you for sharing such wonderful information! In fact when it comes to health, there is nothing more important than managing to eat healthy food and doing exercise regularly.
ReplyDeleteFINALLY FREE FROM HERPES VIRUSI thought my life had nothing to offer anymore because lifebecame meaningless to me because I had Herpes virus, thesymptoms became very severe and bold and made my familyrun from and abandoned me so they won't get infected. I gaveup everything, my hope, dreams,vision and job because thedoctor told me there's no cure. I consumed so many drugs butthey never cured me but hid the symptoms inside me makingit worse. I was doing some research online someday when Icame across testimonies of some people of how DR Ebhotacured them from Herpes, I never believed at first and thoughtit was a joke but later decided to contact him on the detailsprovided and when I messaged him we talked and he sent mehis herbal medicine and told me to go for a test after twoweeks. Within 7 days of medication the symptomsdisappeared and when I went for a test Lo and behold I wasNEGATIVE by the Doctor Who tested me earlier. Thank you DREbhota because I forever owe you my life and I'll keep ontelling the world about you. If you are going through samesituation worry no more and contact DR Ebhota viadrebhotasolution@gmail. com or WhatsApp him via +2348089535482.he also special on cureing 1. HIV/AIDS2. HERPES 3. CANCER 4.ALS 5. HEPATITIS B 6.DIABETES 7. HUMAN PAPILOMA VIRUS DISEASE(HPV)8. ALZHEIMER 9. LUPUS (Lupus Vulgaris or LupusErythematosus
ReplyDelete