BOIL THAT WATER, SHE'S GONNA HAVE A BABY!
By Keith Souter, aka CLAY MORE
How many movies have you watched and heard those words? Quite a few, I imagine. Did you wonder exactly what the water was for? I mean, boiling water? Surely not to apply to the mother-to-be? But of course, you never find out because as soon as the water is brought in, the menfolk are rushed out and the expectant mother and her female neighbour, midwife or doctor are left to do their magic. Then you see the anxious father pacing up and down, acting clumsily or irrationally as he awaits that slapping noise, which was always followed by the cry of a newborn babe. Then the door opens and either a neatly wrapped baby is presented to the father or he is ushered in to see his wife with the baby ready for the proud father to see.
WARNING! THE REST OF THE ARTICLE IS GOING TO LOOK AT CHILDBIRTH, A SUBJECT THAT STILL MAY CASE FOLKS SOME ANXIETY. IF YOU ARE OF AN ANXIOUS DISPOSITION THEN READ NO FURTHER.
A natural birth
Nowadays most fathers attend antenatal classes and so they have a good idea of what is happening throughout the pregnancy. They know what to expect when labour begins, what they need to do, and a lot of fathers are present during the birth of their children. Some may been have delivered the baby themselves.
In the 19th century things were very different. Fathers didn't tend to have much to do with the pregnancy, apart from the obvious conception, of course. Most women received no antenatal care. When they went into labour they may have just gone somewhere on their own and given birth, or may have had a willing relative or neighbour that they could have help from. The father may have kept on working the land. A day or two after the birth she may have been back there helping him. Interestingly, this is still pretty much what happens in rural areas in the developing world.
Explanation of the birth mechanism from Fleetwood Churchill's 'On the Theory and Practice of Midwifery,' 1850.
So let's look at what happens
Pregnancy
This lasts 40 weeks, on average. A rule of thumb for calculating the expected date of delivery (EDD) is to take the first day of the last menstrual period (LMP) and add seven days, then subtract 3 months. This is working on the basis of conception occurring about two weeks before that, when ovulation, or the release of the egg from the ovary occurs.
During the first twenty weeks the baby is developing. During the second twenty weeks the baby's organs have all developed and it grows.
Another rule of thumb - the average mother will put on 28 pounds in pregnancy, 8 pounds only in the first 20 weeks, then a pound a week until term (ready to give birth).
Labour
There are three stages of pregnancy:
First stage - from the onset of contractions until the mouth of the womb (uterus) has opened up fully enough to allow for delivery. This can take 12-16 hours in a primiparous womb (first timer), but only 6-8 hours in a multiparous (a mother having had at least one previous pregnancy).
Second stage - the birth of the baby. This lasts 3-4 hours in a primiparous women, but may be very fast in a multip.
Third stage - the delivery of the placenta, or afterbirth. It usually comes away within half an hour of the birth of the baby.
After the baby is born the cord is ligated and separated. This is done a few inches from the umbilicus. This umbilical stump will gradually shrivel and separate after a few days. It used to be advised to cut quickly, but modern research suggests that waiting until the placenta has delivered gives a premature baby more blood and more stem cells, all of which is better for them.
Complications
While the majority of pregnancies do go through to an uncomplicated labour and birth of a child, yet there are still a considerable number that have complications. There can be problems with the baby as the result of failure to develop one organ or another. The result can be miscarriage, when nature ends the pregnancy or stillbirth of a dead baby, or birth of a baby with a congenital malformation.
There can be problems with the pregnancy itself; for example, difficulties with the mother's blood pressure, which can lead to kidney failure, convulsions and even death. Nowadays we are familiar with pre-eclampsia, toxaemia of pregnancy and the various related problems, but back in the mid-nineteenth century there was no conception about blood pressure, so no way of helping.
Then there can be problems about the position of the placenta. If it is too low, which we call placenta praevia, then this can produce hemorrhage either before labour or during labour if it detaches from the uterine wall.
The cord can prolapse during labour. That means it can come out before the baby and the baby's own head can therefore obstruct its own blood supply.
And there can be problems about going over term, or just not progressing during the labour. These are things that we can do a lot about nowadays, but back then there were a limited number of drugs and herbs that could be used. [I'll be looking at herbs and drugs in a later blog.]
Multiple births
Twin and triple pregnancies occurred and would challenge whoever was assisting the mother. These are more likely to be difficult labours and there is a lot of potential for things to go wrong with both babies. You may think that if a baby is born quickly then all will be well. Not necessarily. If a baby is born too quickly there can hemorrhage into the baby's brain.
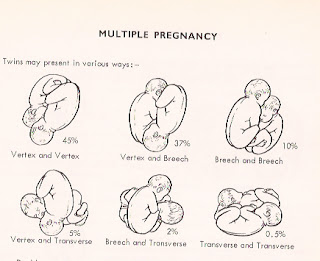
Twins presentation in The Rose Garden, a 1513 publication for midwives
And of course, there can be problems from the twins' positions. Caesarian sections would not have been a ready option and a good midwife or doctor would be essential.
Good old Doc Adams was adept at delivering babies and looking after the newborn. Indeed, in The Baker's Dozen, from Gunsmoke's season 13, in 1967, he is involved in the aftercare of triplets who were born to a woman who arrived in Dodge City on a stage that had just been robbed. The mother sadly dies in the process, and it transpires that the father was a stage robber who has been killed. Doc looks after the triplets and is determined that they should be kept together and not sent to the State orphanage.
Malpresentations
When we assess a mother's abdomen we talk about the presentation. That means the anatomical part of the baby that is leading and which is likely to be born first. There are whole number of ways that we refer to them - cephalic, meaning the head first. This is the one we always want to find. There are variations, of course, so you can have vertex (top of head), sinciput (forehead), face, chin, occiput (back of head) and others.
Other presentations are called malpresentations. Thus a foot, a shoulder, a hand or a bottom (breech) all present difficulties for the doctor or midwife. Indeed, nowadays with good antenatal care you aim to know precisely how a baby is lying well in advance of the due date and plans can be made. This may well be a planned Caesarian Section. Back in the 19th century there were no scans, everything had to be worked out through clinical acumen alone and the use of a simple foetal stethoscope.
The author's foetal stethoscope - which is more or less obsolete today, since most doctors have an ultrasound gadget
A breech presentation occurs in about one in every 40 cases. It is a common position early on in about a quarter of pregnancies, but a fair number will turn round before the critical 36 weeks stage. In the 19th century the first inkling of this would probably be at term, when the woman was going into labour. Again, nowadays we would aim to know well ahead and plans would be made.
External cephalic version is the name of the technique used in trying to turn a baby from the outside. It would be done from 32 weeks to 35.
External Cephalic Version - an attempt to gently turn the baby from breech to cephalic presentation in advance of term
The instruments
Most frontier doctors would carry obstetric instruments with them. That is they would have obstetric forceps to help to deliver the baby's head when it is is in the vagina and effect delivery by traction without causing injury.
There are several types, but the common features are the two curves. They have a cephalic curve to be applied to the baby's head, and they are have a pelvic curve to fit the pelvic curve of the birth canal.
Not only would a doctor carry forceps, but he would have instruments to perform an episiotomy, an incision needed to allow room for the forceps and often also to give a baby enough room to get out. He would also have to have sutures and instruments to repair the episiotomy.
Yet sadly, he would also have to carry other instruments in case things had gone wrong and the baby had died. I think that is as far as I need explain, but if anyone would wish for further information, then I can be contacted off-line.
Sepsis - the great killer
At this point we really have to talk about maternal mortality. Here I am going to talk about the situation in the UK, since I am more familiar with it and have figures. I believe that the points are still germane when applied to the USA and the frontier.
At the beginning of the 19th century pregnancy and childbirth carried significant risks for the health of a woman. One in 200 women died in childbirth. In part this was to do with complications of being poor, of not having enough money for food. Rickets, due to vitamin D deficiency caused skeletal problems and pelvic distortions, so labour could be difficult and become obstructed with catastrophic results for mother and child.
Yet the maternal mortality in hospitals was actually greater! That is right, you had a higher risk if you went into hospital for treatment. They did not realise it, but the problem was puerperal fever - which they recognised - but they still did not understand the problem of sepsis.
In fact, a Scottish physician, Dr Alexander Gordon, working in Aberdeen had made the link at the end of the 18th century when he deduced that there was a connection between puerperal fever and erysipelas (an infection later found to be due to Streptococcus). He wrote a treatise about it, but it had no impact. He drew a significant conclusion and stated that he believed that somehow doctors and midwives spread the problem. Yet along with his fellow physicians he advocated that the treatment should be venesection or bleeding.
Oliver Wendell Holmes (1809-1894), a doctor, poet and writer, sometime dean of Harvard Medical School, also made the connection and suggested that doctors in particular were the problem. He went so far in a paper of 1843 to suggest that doctors who conducted autopsies should not also practice obstetrics.
Professor Oliver Wendell Homes
Yet history proclaims Ignatz Semmelweis (1818-1867) as the man who made the breakthrough. He published a treatise in Budapest in 1861, entitled ‘The Cause, Concept and Prophylaxis of Puerperal Fever.’ It was based on work he conducted in the 1840s. He suggested that women who died from puerperal fever (childbearing fever) had been contaminated by doctors who had not washed their hands between attending morning autopsies and going to the labour wards. He was castigated by his fellow practitioners for daring to suggest that they should wash their hands, without any 'scientific evidence' as to why. It was said that he was not saying anything new, it was just the same thing that Holmes had been saying.
He actually suffered a nervous breakdown and was committed to an asylum in Vienna, where he died a fortnight after his committal, after having been beaten by guards.
These are operations performed to remove the child from the mother's womb through an incision in the abdomen. They first one to be done in which the mother survived was in Ireland in 1738. The first in England was performed by Dr James Barlow in 1797 and the first in the USA was by Dr John Richmond in 1827. These were all done without anaesthetic and so when anaesthesia became generally used, together with aseptic surgical techniques, Caesarian Sections became viable operations.
In the 1880s the classical Caesarian Section method was developed, which involves a longitudinal incision in the upper uterine segment. That is, in the upper part of the womb. These do not heal well, so they were replaced in 1906 by the lower segment Caesarian section. This is the method favoured today, although under certain situations the classical may be performed.
So what about that boiled water?
Well, it would be useful. Not only to sterilise as best one could the instruments, but also to use to make warm(not booing) compresses to place over the perineum prior to labour. This would tend to soften the tissues, which get stretched, of course, and lessen pain and reduce tearing of the tissues.
And of course, it would be for washing hands and swabbing everything down afterwards. On the point of washing hands, it should be noted that the frontier doctor's hands would probably have a greater need of being washed than would a midwife. Quite simply, the midwife would not be handling purulent matter, operating on diseased tissue or conducting autopsies. Nor would she have been exposed to coughs and sneezes to the same extent as the doctor.
And that slap on the back?
Well, we don't do that any more either. Doctors and midwives used to do it to stimulate the baby, in the belief that you needed it to help it to breathe and to cry to clear all those secretions out of nose and mouth. Now we just suck it out with a tube and if needed, give controlled oxygen.
A couple of final points about cutting the cord
This is really if you ever find yourself having to deliver a baby. Don't go searching for a scissors of anything else to cut that cord. nature generally does a good job. Don't cut it, or tie it off, just call the emergency services and let them clamp it off for you. As noted above, a slight delay is no bad thing, and may be quite beneficial to the baby.
Lastly, any cutting of a cord has to be done with a clean instrument. I say this from experience of many moons ago, when I was working in a fever hospital in India. There was a whole ward devoted to cases of neonatal tetanus. Almost all of them had been due to injudicious severing of the cord with any sharp object hat was at hand- knives, scissors, sickles!
Tetanus or Lockjaw is a horrid condition - which I'll be getting round to at some stage.
__________________________________________________________________________
Hell on the Prairie, the sixth Wolf Creek book features Keith (Clay More's) character Dr Logan Munro, the town doctor in THE OATH, a story about a spectre from his past. Logan has been in Books 1, 4 and 6, and is due to appear in books 8 & 9.
And his other new character, Doc Marcus Quigley, dentist, gambler and occasional bounty hunter continues in his quest to bring a murderer to justice, in AMBUSH AT DEAD MAN'S RAVINE, the fourth in his monthly ebook short stories THE ADVENTURES OF DOCTOR MARCUS QUIGLEY published by High Noon Press.
Vol 5 THE SHOOTER should be out soon.













Very interesting. Thanks for taking the time to impart your knowledge on us. :)
ReplyDeleteKeith, thanks for such a comprehensive explanation. The next time I see a movie where someone calls for boiling water, I'll know "the rest of the story."
ReplyDeleteMy pleasure, Jo. Thanks for stopping by.
ReplyDeleteThanks, Tom. And of course, tea is needed for doctor, midwife and newly delivered mother.
ReplyDeleteKeith, I was not in the room when my wife had our children. I think that I am glad. I believe I had a shot of redeye afterwards. I am enjoying your Dr. Marcus Quigley series.
ReplyDeleteJerry
Always good advice from The Doctor's Bag! I'm sure that if I ever do have my characters run into an expectant mother, I'll know exactly what to have happen.
ReplyDeleteHi Jerry, yes, you have to wet the baby's head, so to speak. That's a custom on this side of the pond, at any rate. Not literally wetting the baby's head, but celebrating with a drink.
ReplyDeleteHi J.E.S. Always a well to be prepared. But I guess most cowboys will have an idea about births.
ReplyDeleteOh Keith - what a great post. I had a great-aunt who died of blood poisoning or fever in 1918 or so after childbirth. My mom went to the hospital, although my grandmother had all her births at home. And me? My daughter and I would have both died if not for C-section. Hubby watched, I wanted the sheet. LOL can't stand blood or needles. Can't even see stuff on TV that's fake.
ReplyDeleteJerry, thanks for that. I meant to say that i really enjoyed Charlie's Money.
ReplyDeleteHi Meg, sorry to hear about your great-aunt's death. Yes it is a wonderful operation when it is done as an emergency. It may mean a shortened labour, seeing one's baby sooner and it heals well, generally. Also, there is no episiotomy wound to be sutured and healed.
ReplyDeleteMy dad delivered my little brother at home. No, it was not planned. Mom was paralyzed from the waist down due to a spinal block gone wrong when I was born, so when she went into labor, she didn't know it. Anyway, he delivered the baby, I called the egg lady (the only number I knew), and she and the doctor were there within minutes of the birth. (The doctor had to drive 30 miles, so you know he didn't adhere to the speed limit.) My brother was weighed on chicken scales (9lbs 15-1/2oz), and after everyone left, my dad said that it was easier than pulling a calf.
ReplyDeleteHi Jacquie, well done your dad! I love the fact that your brother was weighed on the chicken scales. What a great story.
ReplyDeleteFascinating stuff. I remind myself that I have modern medicine to thank for my beautiful daughter in law and her children, who came via C-section. Back in the day she would have died the first time. Thanks for a great blog.
ReplyDeleteHi, thanks for stopping by. I am glad that you are enjoying your grandchildren. Nature always does the best that it can, but sometimes we have to give it a helping hand. Yet it is still nature that heals in the end.
ReplyDeleteThank you for your kind words.
Keith
Hi Keith,
ReplyDeleteI'm sorry I am late getting here--I've been out of pocket most of the day. What a wonderful, fascinating post, as always. Like Meg, I had C-sections. My oldest was early and I was in labor for 22 hours--I was so ready for the C-section, let me tell you. LOL I'm very very glad for hospitals. Can't imagine going through childbirth back in those times. Great post, as always!
Cheryl
Terrific post. Whenever I read about childbirth, I find myself in disbelief that I did it twice LOL. Easier being a gramma.
ReplyDeleteThe term antenatal was a new ne for me. Thanks!
Wonderful post, Keith. And thanks for sharing your story Jacquie.
ReplyDeleteOne thing boggles my mind, that doctors wouldn't wash up after an autopsy. Washing hands is taken for granted now. Sure, kids and some adults have to be reminded from time to time, but we all know we should wash our hands. I know, they didn't know about germs then. Regardless, if I'd been doing an autopsy, I'd want to wash my hands just out of general fastidiousness.
(Not to mention death cooties. ;))
I always thought the point of sending the incipient father to boil water was to get him out of the doctor's way.
ReplyDeleteAs I had said earlier, my father was born at home 3 months premature and weighing 2lbs. 9 oz. They kept him going by putting him in a shoe box on the oven door and giving him a shot of whiskey every hour. Your post filled in the rest of the story. Doris
ReplyDeleteHi Cheryl, hospitals are so important, but back in the 19th century they were not always the best place to be born. The maternal mortality rate was higher in hospitals than when folks had home births.
ReplyDeleteNowadays we are seeing another problem with MRSA, or methicillin (a type of penicillin) resistant Staphylococcus aureus, due to the overprescribing of antibiotics and the introduction of antibiotics into the food chain. Unless we can produce other antibiotics or develop different strategies to deal with infections we face a return to 19th century problems with infections.
The simple fact is that we are witnessing evolution within our lifetimes. Essentially, we have created a hazardous environment to the microbial world. They are adapting by developing antibiotic resistance. It is happening incredibly quickly by our standards, since we measure time in years and against our life spans. A microbe's lifetime is much shorter and so a decade is rather like a millennium in the microbial world. The antibiotic resistance is their adaptation, so it cannot be undone.
Hi Tanya, thanks for stopping by. Yes, just like being a grandpa!
ReplyDeleteAnte is Latin for 'before', so antenatal is before birth. Similarly anterior is 'more in front.'
Doctors used to use a number of Latin terns in writing prescriptions, and a number of them are still used, but just as abbreviations. For example, a.c, stands for ante cibos, meaning before food. That is when you want a drug to be taken on an empty stomach to enhance absorption.
But thank you, you have given me an idea for another blog!
Hi Alison, yes, it is hard to believe that folks didn't wash their hands. They just wiped them. Surgeons wore aprons and prided themselves on how 'work-smeared' they got. The germ theory was a fantastic breakthrough, yet it took a long time to persuade many doctors to change their habits. Semmelweis was castigated for having the temerity to suggest that doctors should wash their hands.
ReplyDeleteHi Shay, thanks for stopping by. That is undoubtedly a good and valid point.
ReplyDeleteHi Doris, gosh, that is so light. And putting him in a shoebox and giving him whiskey! What a fantastic story.
ReplyDeleteThat weight suggests that he was really early. When babies are very early, born at 28-32 weeks, they are liable to get respiratory distress syndrome, which is very dangerous. This is because they don't have enough of a substance called 'surfactant' in their airways. It is essentially a lubricant so that their developing airways don't stick together. To be born that early in the old west would have had a high mortality rate, so anything after 32 weeks would be needed to get a fighting chance.
Very informative post.
ReplyDeleteEarly in my career I worked in labor and delivery. When all went well, it was a happy and joyful place to be, but if something went wrong or we lost a baby or a mom, it was the worst job I could ever imagine.
Even in the modern world, disease is spread by the lack of handwashing. I was amazed by the tetanus following the cutting of the cord with random instruments in India. How horrible.
This is great information for writers. I always enjoy your posts.
Thanks, Keith. Will definitely be useful down the line. I tend to use knowledgable old women of indeterminate background with an encyclopedic knowledge of medicinal herbs and helpful native practices. But soon I'll get around to a frontier doctor.
ReplyDeleteThanks, Sarah.
ReplyDeleteI agree, a great experience when all goes well. In my early career we still did home confinements and they were always a bit anxiety-provoking, but fortunately, they all had satisfactory and satisfying results.
Hi Charlie, I'm all in favour of the wise old woman who has seen and done it all. As I mentioned, in the days of the early hospitals a woman may well have fared better in the old wise woman's care.
ReplyDeleteThanks for an enlightening post, Dr. Souter. I always wondered what the heck the hot water was for in the days before antisepsis.
ReplyDeleteI read Evan Hunter's book "The Cry And The Covenant", about Ignatz Semmelweiss, many years ago. Interesting to learn that others also came up with the same 'crazy' idea of washing the hands.
I wonder if you could enlighten me of a fact re Caesarians. They're named after old Julius, of course, and the encyclopaedia says he was probably delivered this way. In the first century B.C., and his mother was still alive when he was a mature man. Just curious.
My dad and his seven siblings were born to a diabetic mother from 1912 to 1925 and all weighed, of course, more than normal new babies, from 12 to 14 pounds. Two others died, apparently from some complication. My paternal grandmother died in 1956 from complications of diabetes aged 65. This was, by the way, in urban Australia.
My husband's father, on the other hand, was born weighing 3 pounds in 1908, the eldest of ten. He was of much the same build as my dad and lived into his early eighties; my father died of kidney failure at 73 years and 10 months. His was the youngest passing-on in his family, all of whom survived to their eighties and nineties, one 99, and one is still with us.
I'm glad we were all born into a much safer modern world. Though when I had my first two children in 1960 & 1962 one wasn't anaesthetised until the head presented. Much better case with the last two with laughing gas.
Thanks again for your post.